2894
Views & Citations1894
Likes & Shares
Highly active antiretroviral therapy has enabled people with HIV to live longer and have more productive and satisfying lives. An individual diagnosed with HIV at age 20 can expect to live into his/her early 70’s. The de-classification of HIV from an acute to a more manageable chronic disease in which people living with HIV can now manage this disease on their own is attributed, in part, to the success of this therapy. The author proposed a self-management framework that clinicians can use to identify potential barriers that may circumvent their patients from achieving a favorable distal outcome in this framework or obtaining viral suppression at the last step of the HIV care continuum. By adopting a treatment modality that utilizes this framework, clinicians can make a great contribution to the United States government’s 2019 initiative to end the HIV epidemic within 10 years by addressing two key strategies to achieve this desired outcome.
Keywords: HIV, Highly active retroviral therapy, Self-management framework, Ending the HIV epidemic
INTRODUCTION
Highly active antiretroviral therapy (HAART) is a revolutionary breakthrough for people living with HIV. A critical change that HAART, which is the use of a combination of HIV medicines called a HIV regimen, has brought about is that there is an increase in the life expectancy for people on HAART. Research by Harrison et al. [1], using population-based HIV surveillance data from 25 states in the United States, found that life expectancy after a HIV diagnosis improved significantly from 10.5 years in 1996 to 22.5 years in 2005, which means that the life span doubled during this time. There was a particular rise in life expectancy in the first 5 years after the introduction of HAART.
More promising, research by Samji et al. [2] in their study of participants from the North American AIDS Cohort Collaboration, found that a 20 year old HIV-positive adult on HAART in the United States or Canada would be expected to live into their early 70’s. This life expectancy estimate approaches that of the general population in these countries. The life expectancy gap between HIV-positive and HIV-negative persons is closing. Marcus et al. [3] found in their Kaiser Permanente California study that for 20 year old HIV-positive persons on HAART, there was an 8 year gap in life expectancy compared with their HIV-negative counterparts.
A second major change that HAART has brought about is that HIV has been de-elevated from an acute to a more manageable chronic disease [4]. Many people living with HIV are now able to provide their own care through disease-specific care that includes behaviors directed to symptom management and medication adherence and generic care that involves health maintenance types of behaviors like managing any psychological distress that may arise and addressing the nutritional needs that are associated with this disease [5,6].
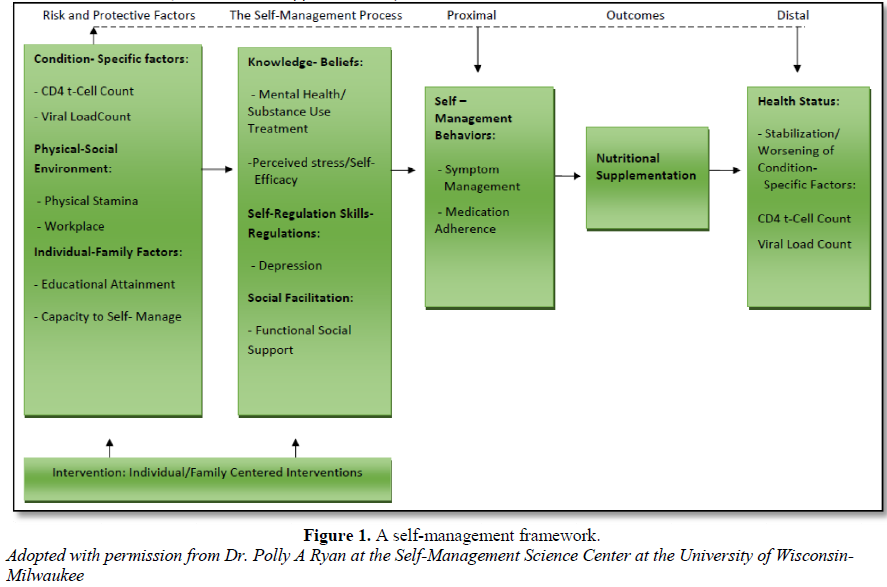
A self-management framework is presented in Figure 1 that can be used to guide clinicians in helping their patients to manage HIV. This framework is composed of Risk and Protective Factors (condition-specific factors - CD 4 T-cell count, viral load count; physical-social environment factors - physical stamina, workplace; individual-family factors - education attainment, capacity to self-manage), self-management process variables (knowledge/beliefs-mental health care and substance-use treatment, perceived stress-self-efficacy; self-regulation skills-depression; social facilitation-functional social support), Proximal Outcomes (self-management behaviors - symptom management, medication adherence; nutritional supplementation) and Distal Outcomes (health status - stabilization/worsening of condition-specific factors - CD4 t-cell count, viral load count). The reader is referred to Ellis [7] for a detailed description of this framework.
THE HIV CARE CONTINUUM AND SELF-MANAGEMENT FRAMEWORK
The United States Centers for Disease Control and Prevention (CDC) tracks HIV using a series of steps from the time a person receives a diagnosis of HIV, linked to care, received or were retained in care and has become virally suppressed. Viral suppression is measured as a viral load test result
The self-management framework through its risk and protective factors, self-management process variables and proximal outcomes provide feedback to clinicians as to potential barriers in the received or retained in care step of the HIV care continuum that may prevent their patients from achieving a favorable distal outcome in this framework or reaching viral suppression in the last step of this continuum. In this framework, self-management process variables-mental health care and substance-use treatment and cognitive-affective depression, have all been found to increase the need for nutritional supplementation among seropositive mothers [7]. This was found to be a barrier for many of these resource-constrained mothers because the nutritional supplements that were prescribed to them were over-the-counter (OTC) products, and had to be paid for out-of-pocket because the Medicaid Program in North Carolina did not provide coverage for the types of OTC products that these mothers were in need of; multivitamins, minerals, and nutritional drinks. This Medicaid policy and it continues to be in place in this state along with 7 other states that do not provide this Medicaid benefit at all [10,11] and inability of resource-constrained people living with HIV to pay out-of-pocket or borrow money from their family members or friends to buy these OTC products to complement HAART circumvent them from achieving a favorable distal outcome in the self-management framework and reaching viral suppression at the last step of the HIV care continuum. This finding is important because the CDC [12] reported that in 2016, 11% of people living with HIV and receiving care were not virally suppressed, accounting for one-fifth new transmissions during this time period.
CONCLUSION
People living with HIV on HAART are experiencing longevity in the life course. This is so promising that in President Donald J Trump’s State of the Union Address on February 5, 2019, it was announced that the goal of his Administration is to end the HIV epidemic within 10 years [13].
This initiative includes 4 key strategies:
1. Diagnose all people with HIV as early as possible.
2. Treat people with HIV rapidly and effectively to reach sustained viral suppression.
3. Prevent new HIV transmissions by using proven interventions, including pre-exposure prophylaxis (PrEP) and syringe services programs (SSPs).
4. Respond quickly to potential HIV outbreaks to get needed prevention and treatment services to people who need them.
By adopting a treatment modality that utilizes the self-management framework in Figure 1, clinicians would be able to identify barriers while their patients are in care that could potentially hinder them from achieving strategy 2 in the government’s goal to end the HIV epidemic. At the same time, strategy 3 will be met because with an undetectable viral load HIV is untransmittable [8,9,14].
1. Harrison KM, Song R, Zhang X (2010) Life expectancy after HIV diagnosis based on national HIV surveillance data from 25 States, United States. J Acquir Immune Defic Syndr 53: 124-130.
2. Samji H, Cescon A, Hogg RS, Modur SP, Althoff KN, et al. (2013) Closing the gap: Increases in life expectancy among treated HIV-positive individuals in the United States and Canada. PLoS One 8: e81355-e81367.
3. Marcus JL, Chao CR, Leyden WA, Xu L, Quesenberry CP Jr, et al. (2016) Narrowing the gap in life expectancy between HIV-infected and HIV-uninfected individuals with access to care. J Acquir Immune Defic Syndr 73: 39-46.
4. Gifford AL, Groessl EJ (2002) Chronic disease management and adherence to HIV medications. J Acquir Immune Defic Syndr 31: S163-S166.
5. Barlow J, Wright C, Sheasby J, Turner A, Hainsworth J (2002) Self-management approaches for people with chronic conditions: A review. Patient Educ Couns 48: 177-187.
6. Chou FY, Holzmer WL (2004) Linking HIV/AIDS clients’ self-care with outcomes. J Assoc Nurses AIDS Care 15: 58-67.
7. Ellis WL (2015) An analysis of a self-management framework to identify factors affecting the need for nutritional supplementation among seropositive African-American mothers. J HIV AIDS 1: 1-8.
8. The United States Centers for Disease Control and Prevention (2019) Understanding the HIV care continuum. United States Government Printing Office, Atlanta, GA.
9. UNAIDS Explainer (2018) Undetectable-untransmittable: Public health and HIV viral load suppression. UNAIDS, Geneva, Switzerland.
10. The Henry J. Kaiser Family Foundation (2018) Medicaid benefits: Over-the-counter products. The Henry J Kaiser Family Foundation, San Francisco, CA.
11. Ellis WL (2012) Perceived stress levels among HIV/AIDS-infected mothers: The role of over-the-counter products. Soc Work Health Care 51: 850-867.
12. The United States Centers for Disease Control and Prevention (2019) Gaps in HIV testing and treatment hinder efforts to stop new infections. United States Government Printing Office, Atlanta, GA.
13. Department of Health and Human Services, USA (2019) What is ‘ending the HIV epidemic: A plan for America’? Ending the HIV Epidemic.
14. Eisinger RW, Dieffenbach CW, Fauci AS (2019) HIV viral load and transmissibility of HIV infection: Undetectable-untransmittable. JAMA 321: 451-452.
QUICK LINKS
- SUBMIT MANUSCRIPT
- RECOMMEND THE JOURNAL
-
SUBSCRIBE FOR ALERTS
RELATED JOURNALS
- Oncology Clinics and Research (ISSN: 2643-055X)
- Journal of Clinical Trials and Research (ISSN:2637-7373)
- International Journal of Surgery and Invasive Procedures (ISSN:2640-0820)
- International Journal of Anaesthesia and Research (ISSN:2641-399X)
- Journal of Cell Signaling & Damage-Associated Molecular Patterns
- Journal of Immunology Research and Therapy (ISSN:2472-727X)
- Journal of Forensic Research and Criminal Investigation (ISSN: 2640-0846)