3370
Views & Citations2370
Likes & Shares
A case describing the successful rehabilitation of a patient with a right homonymous hemianopia field loss is presented. The patient was fitted with binocular 20-dioptre Palomar prisms, following a 2 month trial with Fresnel prisms. The patient had a total restitution of the central field, thus improving their quality of life. In no case was exotropia or central scotoma of field of vision (FoV) presented with the binocular prisms as other authors refer. Exact calculation of the prism power was made between the empirical calculation and the trial lens prisms facilitated the determination of the position of the prisms by means of a calculation of trial and error. We compare the results obtained with what other authors refer.
Keywords: Homonymous hemianopia, Visual rehabilitation, Palomar prisms, Loss of visual field
INTRODUCTION
Patients with normal visual acuity and complete homonymous hemianopia (CHH) present spatial orientation difficulties that negatively impact their quality of life. They can lose the ability to dress themselves, may ignore routes that are familiar, stumble when walking alone, collide with obstacles and find it all but impossible to read or work with a computer. In short, they lose personal autonomy [1,2].
Homonymous hemianopia (HH) is a disorder of the visual field with loss of vision in both monocular hemifields, contralateral to the side of brain injury [3,4]. The prevalence of HH is of approximately 0.8% in the general population older than 49 years [5], with about 2 million stroke survivors in rehabilitation suffering from either HH or hemineglect in the United States annually [6,7]. Homonymous hemianopias from post-chiasmatic visual pathway injuries are primarily caused by posterior cerebral artery infarction and, to a lesser extent, by head trauma, tumors and surgery [8-11].
Patients diagnosed with HH, even with fair distance and near visual acuity, complain of significant difficulties in their daily activities, including inadequate mobility, frequent collisions with unseen objects, and other limitations in such tasks as shopping, financial management, telephone usage, meal preparation [12,13] and driving [14]. Reading is particularly affected by the visual loss that accompanies HH, with a reduction in reading speed, an increase in visual omissions and guessing errors and an alteration in the pattern of ocular movements as the most frequently documented symptoms of hemianopic dyslexia [9,15].
There is a small body of scientific literature [16-19] reviewing the factors associated with the epidemiology, an etiology, clinical presentation and course of hemianopias. Regarding an etiology, hemianopic defects are among the most common disorders after strokes. Rossi et al. [7] reported that in the USA there were about 10 million cases of head injuries annually, 20% of which were associated with brain injuries, and that a third of patients who survived a stroke had complete or incomplete homonymous hemianopia (HH).
Gottlieb et al. [21] examined the use of 15-diopter plastic press-on Fresnel prisms as a means of recovering the FoV in 18 patients with stroke and homonymous hemianopia or unilateral visual neglect. After four weeks the prism-treated group performed significantly better than controls on several tasks requiring hand-eye coordination. The authors concluded that the treatment with 15-diopter Fresnel prisms improves visual perception test scores, but not the performance on the Barthel ADL test [22], in stroke patients with homonymous hemianopia or unilateral visual neglect.
Gottlieb et al. [21], Zihl [23] and also Kasten et al. [24] suggested that regular training of the blind FoV using visual stimuli similar to those used in a computer-controlled perimetry test could facilitate recovery of the FoV next to the midline and provide an expansion of the FoV.
Pambakian and Kennard [20] addressed the issue of whether it was possible to restore visual function in patients with CHH. They emphasized the importance of several rehabilitation treatments, such as psychophysical techniques, for improving care in the blind half of the FoV. They also suggested the possibility of using optical aids, hemianopic mirrors and prisms, as well as cognitive techniques for improving eye movements. They concluded that research on rehabilitation of patients with brain damage and functional impairment was a very difficult and laborious task. In addition, they acknowledged that the effectiveness of such treatments was not properly detailed, since there was insufficient research and most published studies suffered from some methodological flaw.
In a comprehensive review, Peli [25] classified the effects of the instruments used in the rehabilitation of hemianopia into two groups: those relocating the FoV and those producing expansion. He argues that the expansion effect of the FoV is preferred because the simultaneous FoV is wider and allows the patient to control the environment at all times, thus enabling safer mobility. However, relocation only changes the position of the lost FoV or its relative position with regard to the midline. This author also holds that the FoV changes when viewed through binocular sectors. Since the patient does not see objects in that part of the FoV he or she is less likely to fixate, and therefore a voluntary eye movement is required. Peli [25] points out that in addition to these limitations, patients have an optical loss of FoV in the centre of the FoV caused by the binocular sectorial prism. Peli [26] has also developed a method consisting in a monocular sectorial prism fit on the eye with the side of the defect and limited to the top or bottom FoV or covering both peripheral FoV. This prism has to be placed across the entire width of the lens in order to be effective in all lateral positions of gaze. The prism expands the FoV by promoting peripheral diplopia, producing optically peripheral exotropia, while maintaining bifoveal alignment. Peli [25] stated that this expansion of the FoV can be measured with standard binocular perimetry because it is effective in all positions of gaze, including the primary position. He uses 40-diopter Fresnel prisms, which give a spread of approximately 20° around the midline. However, since the prism only affects the peripheral vision, one could use another prism of greater power.
O’Neill et al. [27] proposed the use of monocular prisms on the side of the complete hemianopia, with bases at the default address. In this way a peripheral exotropia is produced, which achieves the expansion of the FoV. With regard to the success of the rehabilitation process, Palomar-Mascaró et al. [28-30] emphasized the importance of ascertaining the prismatic power, as well as the need to ensure the correct position when attaching the binocular prism to the lens.
Palomar-Mascaró [10] in a large study of 93 hemianopic patients, confirms that the binocular adaptations of sectorial prisms do not produce diplopia or central scotomas as reported by authors such as Peli [25], it also indicates the importance of maintaining binocular vision in these patients and refers to the importance of a precise calculation in the power and centering of the prisms for optimal adaptation. The author says that patients treated with Palomar's attached prisms greatly improve their spatial perception, impacting favorably on their quality of life [10,11,28-32].
REVIEW CASE
For its rehabilitation, we advise to use the adjacent Palomar prism technique, which consists of the binocular adaptation of prism bands. These are 15 mm wide strips, moved 2 mm towards the heminopsic side. The patient did not have central diplopia and was able to totally recover the central visual field, without needing to do any ocular movements to see both sides of the field, being able to walk without assistance [29,31,32].
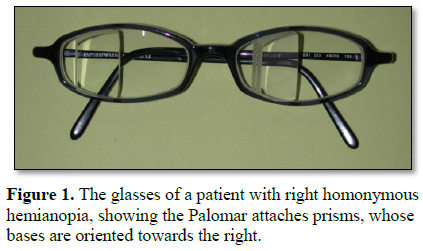
The report describes the binocular adaptation of Palomar prisms in a young patient with right homonymous hemianopia 28. Central visual field restoration, which did not require compensatory eye movements, was achieved through careful selection of prism power from a trial set, while precise prism positioning was essential to avoid central diplopia [17] (Figure 1). The patient did not present in any central diplopia with Palomar prisms adapted binocularly, as described by other authors [10,29,30,33].
It is relevant to mention that whereas precise prism location ensures the smooth transition between both hemifields of view, patients must still perform scanning movements through the prism half of the spectacles in order to observe objects located at the extreme periphery of the hemianopic fields.
The patient of this case, reported an improvement in her ability to perform daily activities, she was walking completely unassisted and she reported being able to watch television and perform near-vision tasks with less difficulty, as well as to successfully interact with various daily life objects. Three years later, the patient has a satisfactory quality of life with no complications with her visual aid.
From our point of view, Palomar prisms are a good option for treatment in cases of complete hemianopsia.
DISCUSSION
Different optical devices have been employed to treat HH patients, either providing a shifting (relocation) or an expansion of the field of view. Although field of view expansion is preferred over relocation, binocular ground-in sectorial prisms only provide image relocation for enhanced peripheral awareness [25]. The effect of binocular sector prisms has been described as being limited [34].
A major problem that urgently needs to be addressed by the visual sciences concerns the extent to which rehabilitation and partial restoration of the FoV is possible in patients with CHH. It is also important to determine whether or not the acquisition of compensatory oculomotor strategies by these patients leads to improvement in their performance and normal functioning [2].
The present study describes the rehabilitation of a young patient with right HH with binocular Palomar prisms, once prism power and location have been determined, in this case we recommend prescribing them as provisional Fresnel prism segments, to be worn for a period of 1 or 2 months in order for the patient to become adjusted to the change in peripheral visual field position [2]. During this time, patients are also instructed to follow a program of daily exercises to facilitate their acceptance of the new optical device. For better optical quality and durability, as well as to provide the same clarity of vision in both hemifields [10] of view, Fresnel prisms are later replaced with Palomar prisms.
The precise adjustment of prism power and location getting reduced disability resulting from the loss of FoV, to increase patients’ confidence and to facilitate reintegration into their social and professional lives by restoring autonomy [2,10,27].
The results from this calculation, which was derived from previous clinical experience with similar cases [10,28,30,32], were later further refined with the aid of trial case prisms and a trial spectacle frame, which also allowed for accurate determination of power prism and your location.
Prism location is critical to avoid diplopia in primary gaze while allowing objects that would normally fall in the hemianopic field to be relocated to the residual field, thus becoming visible in primary gaze [28,29].
Other authors refer that the binocular sectorial prism causes diplopia and a central scotoma in the visual field [26]. The patients don’t find diplopia or the appearance of an exotropia or visual scotoma at any moment, we think this due to is precise placement of the prisms, in addition to doing it binocularly, the patient continues to have binocular vision, which prevents a phoria by prismatic decompensating from appearing [10].
We consider that prism location and the exact calculation of its power is critical to avoid diplopia in primary gaze while allowing objects that would normally fall in the hemianopic field to be relocated to the residual field, thus becoming visible in primary gaze [28,31,35].
For it the evaluation of the 10-degree central field is essential to determine the congruency of the hemianopic lesion, that is, whether the homonymous defects in the fields of both eyes are identical [32], as well as to verify if the lesion follows a straight vertical meridian bisecting fixation between the blind and the normal halves of the visual field [28,30,31].
This results raise the question of how (i.e., through what monocular mechanisms) such spatial reconstruction may occur. There are two possible scenarios that could explain the results. One explanatory hypothesis is based on the recovery of perception corresponding to the central-part FoV of the lost half-retina. This hypothesis assumes that cerebral neuroplasticity processes are induced in the patient and that this enables recovery of alternative visual processing pathways. One obvious way to test this idea would be to obtain neuroimaging recordings of brain regions involved in processing the target location when it is localized in positions corresponding to the lost FoV [2].
CONCLUSION
To conclude, the performance of this study with a large homogenous sample of patients and the results obtained demonstrate the clinical efficacy of binocular Palomar prisms, as a rehabilitation technique, for patients with complete homonymous hemianopia.
1. Egido J, Díez-Tejedor E (2003) Después del ictus. Guía práctica para el paciente y sus cuidadores. Ed. Edide, Barcelona.
2. Palomar Mascaró F, Quevedo Junyent LL, Aznar Casanova JA (2017) Effective visual field rehabilitation in homonymous hemianopia by attaching binocular prisms to lenses. Am Res J Ophthalmol Optometry 1: 1-11.
3. Duke-Elder S (1970) System of ophthalmology. London: Henry Kimpton 5.
4. Harrington D (1964) The visual fields. A text book and atlas of clinical perimetry. 2nd Edn. Saint Louis: Mosby Company.
5. Gilhotra JS, Mitchell P, Healey PR, Cumming RG, Currie J (2002) Homonymous visual field defects and stroke in an older population. Stroke 33: 2417-2420.
6. National Center for Health Statistics (2008) Cerebrovascular disease or stroke. Available at: http://www.cdc.gov/nchs/fastats/stroke.htm
7. Rossi PW, Kheyfets S, Reding MJ (1990) Fresnel prisms improve visual perception in stroke patients with homonymous hemianopia or unilateral visual neglect. Neurology 40: 1597-1599.
8. Zhang X, Kedar S, Lynn MJ, Newman NJ, Biousse V (2006) Homonymous hemianopias: Clinical-anatomic correlations in 904 cases. Neurology 66: 906-910.
9. Zihl J (2000) Rehabilitation of visual disorders after brain injury. Hove, UK: Psychology Press.
10. Palomar-Mascaró FJ (2013) Tesis doctoral: Hemianopsias homónimas completas: Estudio de las técnicas de rehabilitación y calidad de vida. Barcelona. Available at: http://hdl.handle.net/10803/117022
11. Palomar Petit F, Palomar Mascaró FJ, Palomar Mascaró MV (2008) Neurooftalmología. Exploración, pruebas y diagnóstico. Barcelona, Spain: Elsevier-Masson.
12. Romano JG (2009) Progress in rehabilitation of hemianopic visual field defects. Cerebrovasc Dis 27: 187-190.
13. Warren M (2009) Pilot study on activities of daily living limitations in adults with hemianopsia. Am J Occup Ther 63: 626-633.
14. Szlyk JP, Brigell M, Seiple WH (1993) Effects of age and hemianopic visual field loss on driving. Optom Vis Sci 70: 1031-1037.
15. McDonald SA, Spitzyna G, Shillcock R, Wise RJS, Leff AP (2006) Patients with hemianopic alexia adopts an inefficient eye movement strategy when reading text. Brain 129: 158-167.
16. Smith, JL, Weiner IG, Lucero AJ (1982) Hemianopic fresnel prisms. J Clin Neuroophthalmol 2: 19-22.
17. Trobe JD, Glaser J (1983) The visual fields manual: A practical guide to testing and interpretation. Florida: Triad Publishing Company.
18. Shofield TM, Left AP (2009) Rehabilitation of hemianopia. Curr Opin Neurol 22: 36-40.
19. Grunda T, Marsalek P, Sykorova P (2013) Homonymous hemianopia and related visual defects: Restoration of vision after a stroke. Acta Neurobiol Exp 73: 237-249.
20. Pambakian ALM, Kennard C (1997) Can visual function be restored in patients with homonymous hemianopia? Br J Ophthalmol 81: 324-328.
21. Gottlieb DD, Allen CH, Eikenberry J, Ingall-Woodruff SJM (1996) Living with vision loss. Atlanta: St. Barthelemy Press, Ltd.
22. Wade DT, Collin C (1988) The Barthel ADL Index: A standard measure of physical disability? Int Disabil Stud 10: 64-67.
23. Zihl J (1995) Visual scanning behavior in patients with homonymous hemianopia. Neuropsychologia 33: 287-303.
24. Kasten E, Wüst S, Behrens-Baumann W, Sabel BA (1998) Computer-based training for the treatment of partial blindness. Nat Med 4: 1083-1087.
25. Peli E (2000) Field expansion for homonymous hemianopia by optically induced peripheral exotropia. Optom Vis Sci 77: 453-464.
26. Peli E (2008) Peripheral field expansion device. Patent No.: US 7,374,284 B2. Available from: https://www.google.com.ar/patents/US7374284
27. O’Neill EC, Connell PP, O’Connor JC, Brady J, Reid I, et al. (2011) Prism therapy and visual rehabilitation in homonymous visual field loss. Optom Vis Sci 88: 263-268.
28. Palomar-Mascaro FJ, Palomar-Mascaro MV, Cardona G, Quevedo L (2011) Successful rehabilitation of a homonymous hemianopia patient with binocular ground-in sectorial prisms: Considerations concerning prism power and location. Neuroophthalmology 35: 138-143.
29. Palomar-Mascaró FJ, Palomar Mascaró MV, Quevedo i Junyent L, Palomar-Mascaró L (2011) Study of visual rehabilitation techniques in CHH: Press-on prisms, adjacent Palomar´s prisms and lateral-nasal-visor mirror. Neuroophthalmology 35: 68-69.
30. Palomar Mascaró V, Palomar-Mascaró FJ, De Miguel Simó PV, Palomar Mascaró L (2000) Investigación y Actualidad de Ayudas visuales para la rehabilitación de las hemianopsias homónimas laterales completas. Anales Instituto Barraquer 29: 79-99.
31. Palomar-Mascaro FJ (2018) Rehabilitation of left homonymous hemianopia with adjacent palomar prism technique and visual therapy on line. J Intellect Disabil Diagn Treat 6: 31-35. Available at: https://doi.org/10.6000/2292-2598.2018.06.02.1
32. Palomar Mascaró FJ (2009) Estudio sobre la efectividad de los prismas adosados en banda de Palomar en la rehabilitación de las hemianopsias homónimas completas. Universitat politécnica de Catalunya. Treballs acadèmics UPCUPcommons. Available at: https://upcommons.upc.edu/handle/2099.1/6576
33. Palomar-Petit F (1979) Rehabilitación en las hemianopsias homónimas. Arch Soc Esp Oftal 39: 685-694.
34. Giorgi RG, Woods RL, Peli E (2009) Clinical and laboratory evaluation of peripheral prism glasses for hemianopia. Optom Vis Sci 86: 492-502.
35. Woo GC, Mandelman T (1983) Fresnel prism therapy for right hemianopia. Am J Optom Physiol Opt 60: 739-743.
QUICK LINKS
- SUBMIT MANUSCRIPT
- RECOMMEND THE JOURNAL
-
SUBSCRIBE FOR ALERTS
RELATED JOURNALS
- Dermatology Clinics and Research (ISSN:2380-5609)
- Journal of Alcoholism Clinical Research
- Journal of Clinical Trials and Research (ISSN:2637-7373)
- Journal of Spine Diseases
- Stem Cell Research and Therapeutics (ISSN:2474-4646)
- Journal of Forensic Research and Criminal Investigation (ISSN: 2640-0846)
- International Journal of AIDS (ISSN: 2644-3023)