4044
Views & Citations3044
Likes & Shares
CASE HISTORY
A 63-year-old woman with a history of hypertension, hyperlipoproteinemia, angular glaucoma, and without preexisting neurological conditions was admitted to the General hospital in March 2021 due to chest pain, fever, and cough. COVID-19 diagnosis was established by a nasopharyngeal PCR test. Chest x-ray verified bilateral pneumonia followed by pulmonary thromboembolism. The patient was discharged home on day 14, respiratory and hemodynamically stable. Shortly after, the family noted the patient's impaired memory of events that happened before the COVID-19 infection and visual hallucinations. After 10 days of stable physical and mental status, the patient became confused and agitated with auditory hallucinations. Disturbances in attention, cognition, altered awareness, and visual hallucinations aggravated in 10 days before hospitalization at the Neurology department, Novi Sad, Serbia. The patient tested negative for COVID-19 at the admission. Post-acute COVID-19 disease was considered and broad diagnostics were undertaken. Her basic laboratory findings showed elevated CRP. Thyroid hormones, vitamin B12 levels, onco-markers, paraneoplastic and antineuronal antibodies were in the reference range. The biochemistry, cytology, and microbiology of CSF were normal.
Serum/urine immunofixation and electrophoresis were in the average range.
Bacteriological cultures, multiplex viral panel, Treponema Pallidum, and Borrelia Burgdorferi probes were negative in blood and CSF. Oligoclonal IGG and IGM bands were absent in CSF. Blood analysis showed slightly positive: beta2 microglobulin, SLL kappa, lambda chains, anticardiolipin IGG/IGM, anti-B2 Glycoprotein IGG/M, and ANA Hep2 on nucleoplasms. Other immunological abnormalities were not found. Electroencephalography showed physiological activity.
MRI conducted in September 2021 demonstrated FLAIR hyperintensity in the temporo-occipital region showing leptomeningeal contrast enhancement which could suggest meningeal hyperemia, consistent with leptomeningitis/vasculitis (Figure 1).
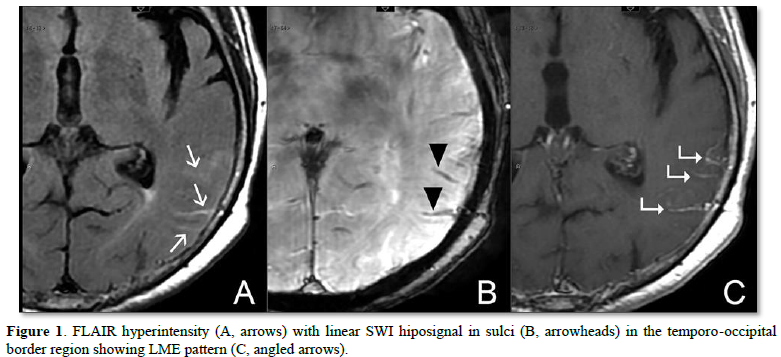
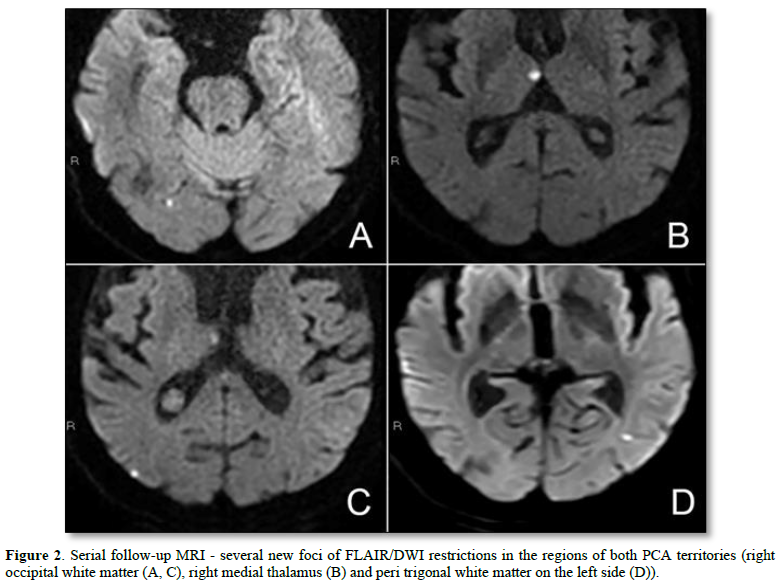
CT angiography and digital subtraction angiography showed no significant abnormalities. Follow-up MRI eight weeks after visualized persistent LME as well as several new foci of diffusion-weighted (DWI) restrictions in the regions of both posterior cerebellar artery territories (Figure 2).
Due to clinical, laboratory, and neuroradiological evaluation without signs of systemic autoimmune disease and malignancy, a COVID-19-CNS vasculitis was suspected. Oral therapy with Prednisolone (40 mg/day) was started with gradual tapering to the daily dose of 10 mg for 6 months. The caregiver reported patient's gradual improvement with mild visual hallucinations, fluctuation of attention and orientation. Consecutive examination defined moderate cognitive impairment with no other neurological signs. Control brain MRI, 6 months after discharge showed resolution of abnormalities. Besides corticosteroid medication, low-dose olanzapine was initiated. After 6 months of the therapy, the patient showed neither behavioral nor cognitive changes and her neurological status was stable.
A possible etiology of post-COVID cerebral vasculitis is an invasion of angiotensin-converting enzyme-2 receptors by COVID-19, leading to endothelitis [6]. The CNS LME on MRI from COVID-19- patients are mentioned in the reports, but the pathology of these lesions remains unclear [7]. Our patient had new-onset neuropsychiatric manifestations after COVID-19 infection. Her first MRI indicative of cerebral vasculitis showed hyper intensive changes in the left temporo-occipital border with a contrast LME pattern. MRI repeated on the 10. day of hospitalization confirmed these changes, as well as new foci of acute microischaemia in the right occipital region and left peritrigonal white matter. According to a metanalysis including MRI findings of 193 COVID-19 patients, there were 27% of patients with LME on contrast MRI, with a greater possibility to have a positive COVID-19 PCR in CSF [7]. The presence of LME in the brain MRI and the severity of COVID-19 were not significantly associated in this study [7]. Literature shows that there is one report of CNS vasculitis confirmed by biopsy in a young woman after COVID-19 infection [3]. One research group presented the case of cerebral and systemic vasculitis with mental alterations beginning 6 weeks after the infection [8]. This clinical presentation and brain MRI findings are similar to our case, yet systemic vasculitis was excluded in our patient. Furthermore, there is a difference in the therapeutic approach in our case in comparison to other cases that reported severe COVID-19 cases demanding intensive support [6]. Our patient was treated with gradual titration of oral corticosteroid therapy for 6 months, consequently with improvement in neurological status, behaviour, and regression of MRI findings.
Neuropsychological examination showed moderate cognitive impairment with memory, attention, and executive dysfunction. According to the literature, COVID-19 patients could encounter global cognitive deterioration and executive function disorders [9]. Del Brutto [10] found a significant reduction in post-pandemic cognitive assessment comparatively to pre-pandemic tests on individuals with mild symptomatic COVID-19 infection [10]. In this case, the altered behavior after COVID-19 infection, brain MRI-leptomeningeal infiltration, without systemic vasculitis- signs, suggest CNS vasculitis after COVID-19 infection. Reported neurological manifestations emphasize the importance of MRI to diagnose complications of COVID-19 brain invasion. Corticosteroids could be efficient in such cases. Further studies about this pathology are needed.
- Fällmar D, Rostami E, Kumlien E, Ashton NJ, Jackmann S, et al. (2022) The extent of neuroradiological findings in COVID-19 shows a correlation with blood biomarkers, Glasgow coma scale score, and days in intensive care. J Neuroradiol 49(6): 421-427.
- Smith CJ, Renshaw P, Yurgelun-Todd D, Sheth C (2022) Acute and chronic neuropsychiatric symptoms in novel coronavirus disease 2019 (COVID-19) patients: A qualitative review. Front Public Health 10: 772335.
- Timmons GM, Rempe T, Bevins EA, Goodwill V, Miner, A, et al. (2021) CNS Lymphocytic Vasculitis in a Young Woman With COVID-19 Infection. Neurol Neuroimmunol Neuroinflamm 8(5): 1048.
- Troyer EA, Kohn JN, Hong S (2020) Are we facing a crashing wave of neuropsychiatric sequelae of COVID-19? Neuropsychiatric symptoms and potential immunologic mechanisms. Brain Behav Immun 87: 34-39.
- Vaschetto R, Cena T, Sainaghi PP, Meneghetti, G, Bazzano, S, et al. (2020) Cerebral nervous system vasculitis in a COVID-19 patient with pneumonia. J Clin Neurosci 79: 71-73.
- Hanafi R, Roger PA, Perin B, Kuchcinski G, Deleval N, et al. (2020) COVID-19 Neurologic Complication with CNS Vasculitis-Like Pattern. Am J Neuroradiol 41(8): 1384-1387.
- Lewis A, Jain R, Frontera J, Placantonakis DG, Galetta S, et al. (2021) COVID-19 associated brain/spinal cord lesions and leptomeningeal enhancement: A meta-analysis of the relationship to CSF COVID-19. J Neuroimaging 31(5): 826-848.
- Ivanovic J, Stojanovic M, Ristic A, Sokic D, Vojvodic N (2022) Post-acute COVID-19 syndrome presented as a cerebral and systemic vasculitis: a case report. Acta Neurol Belg 122(5): 1377-1379.
- Daroische R, Hemminghyth MS, Eilertsen TH, Breitve MH, Chwiszczuk LJ (2021) Cognitive Impairment After COVID-19 Review on Objective Test Data. Front Neurol 12: 699-582.
- Del Brutto OH, Wu S, Mera RM, Costa AF, Recalde BY, Issa NP (2021) Cognitive decline among individuals with a history of mild symptomatic COVID-19 infection: A longitudinal prospective study nested to a population cohort. Eur J Neuro 128(10): 3245-3253.
QUICK LINKS
- SUBMIT MANUSCRIPT
- RECOMMEND THE JOURNAL
-
SUBSCRIBE FOR ALERTS
RELATED JOURNALS
- Journal of Pathology and Toxicology Research
- Journal of Ageing and Restorative Medicine (ISSN:2637-7403)
- Journal of Blood Transfusions and Diseases (ISSN:2641-4023)
- Journal of Otolaryngology and Neurotology Research(ISSN:2641-6956)
- International Journal of Medical and Clinical Imaging (ISSN:2573-1084)
- Chemotherapy Research Journal (ISSN:2642-0236)
- Journal of Allergy Research (ISSN:2642-326X)




