Research Article
Monitoring, Reporting and Evaluation of various Adverse Drug Reactions (ADRs) Under Pharmacovigilance Programme of India (PvPI) in a Tertiary Cardiac Care Hospital, Tamil Nadu
3118
Views & Citations2118
Likes & Shares
Background and Objective: The objective of the study was to monitor, evaluate and analyse various ADRs in a tertiary care hospital and to determine the causality, severity and preventability of reactions.
Methodology: After obtaining approval from Institutional Ethics Committee a prospective observational study was carried out for the period of 12 months (Mar2019-Feb2019). All patients were followed up for ADRs which were evaluated for incidence, frequency, causality, severity, type of ADRs, drug classes, individual drug causing reaction, organ system affected, management and outcome of ADR. Causality was graded according to WHO-UMC scale. Severity according to Modified Hartwig and Siegel scale and preventability based on Modified Schumock and Thornton Scale. Organ System Affected by ADRs were categorized by using IBM Micromedex®.
Results and Discussion: A total of 210 ADRs were reported from 4721 patients during the study period with male (64.2%) predominance over female (35.7%). Most of the reported ADRs were of type A category (87.7%). The class of drug responsible for causing more ADRs was found to be anti-hypertensive (26%) and Diuretics (18%). The most common clinical manifestations of ADRs during the research period was hypokalaemia (11.4%). The most commonly affected organ system was Endocrine metabolic (20%). The suspected ADRs were assessed for their causality, it was revealed that (33.3%) were probable, (64.2%) were possible and (5%) were unlikely. The severity was assessed and observed that (52.8%) were mild, (39%) were moderate and (8%) severe. Preventability of ADR was shown (54.7%) reactions were definitely preventable and (36.1%) reactions were probably preventable and (9%) reactions were not preventable.
Conclusion: Involvement of a pharmacist in patient care can help in prevention and early detection of ADRs, also by detecting new and rare ADRs regulatory decision for the drugs can be made or altered.
Keywords: Adverse drug reaction, Pharmacovigilance, Causality assessment, Severity, Preventability, Spontaneous reporting
Adverse drug reactions (ADRs) are the reaction which causes any unwanted/uncomfortable effects from medication resulting in physical, mental, and functional injuries. The WHO defines an ADR as “a response to a drug which is noxious and unintended and which occurs at doses normally used in man for prophylaxis, diagnosis, or therapy of disease or for the modification of physiologic function” [1].
An ADR is a type of ADE, whose cause can be directly attributed to a drug and its physiologic properties [8]. A main distinction between ADRs and ADEs is that ADRs occur despite appropriate prescribing and dosing, whereas ADEs may also be associated with inappropriate use of the drug or other confounders that occur during drug therapy but are not necessarily caused by the pharmacology of the drug itself [8].ADRs experienced by hospitalized patients are associated with increased morbidity and mortality, prolonged hospitalization, and increased medical expense [5,6]. An increase in the number of drugs on the market, an aging population, and an upward trend in poly pharmacy are contributing factors to the prevalence of ADRs worldwide [2-8].
ADRs has remained relatively unchanged over time, with research suggesting that between 5% and 10% of patients may suffer from an ADR at admission, during admission or at discharge, despite various preventative efforts. The actual incidence of ADRs may be even greater because some ADRs may be undetected or unreported [7,9].
Adverse drug reactions should be quickly identified and managed to limit their effects on the patient. For this reason, several studies have suggested that ADRs are a major public health concern [10,11-15].
CLASSIFICATION
The types of adverse reaction can be explained as “more common ADRs” including type A and B reactions; and “less common ADRs” which include type C, D and E reactions.
ADRs are classified into following categories:
- Type-A: It is the most common type (up to 70%) - Dose dependent, predictable from the known pharmacology of the drug, severity increases with dose. e.g., hypotension by beta- blockers, hypoglycaemia caused by insulin or oral hypoglycaemic or non-steroidal anti- inflammatory drugs induced gastric ulcers.
- Type-B: Rare, idiosyncratic, genetically determined, unpredictable, mechanisms are unknown, Serious, can be fatal; unrelated to the dose, e.g., hepatitis caused by halothane, aplastic anaemia caused by chloramphenicol.
- Type-C: Reaction depends upon the chemical nature of the drug or excipient rather than pharmacological properties. Occurs as a result of continuous drug use. May be irreversible, unexpected, unpredictable, e.g., tardive dyskinesia by antipsychotics.
- Type-D: These reactions occur because of the physical nature of the drug formulation and/or the method of administration. Delayed occurrence of ADRs, even after the cessation of treatment, e.g., corneal opacities after thioridazine, ophthalmopathy after chloroquine, or pulmonary/peritoneal fibrosis by methyserzide.
- Type-E: These reactions are pharmacologically predictable and also known as withdrawal reactions. Occurs typically with the depressant drugs, e.g., hypertension and restlessness in opiate abstainer, seizures on alcohol or benzodiazepines withdrawal; first dose hypotension caused by alpha-blockers (Prazosin) or ACE inhibitors.
- Type-F: These reactions occur only in susceptible patients or individuals with genetically determined, inherited metabolic disorder. Results from the ineffective treatment (previously excluded from analysis according to WHO definition), e.g., accelerated hypertension because of inefficient control [16,17-20,50].
CLASSIFICATION OF ADR BASED ON ITS SEVERITY
The severity of a ADR can be categorized into 4 which are mild, moderate, severe and lethal.
- Mild adverse reactions are those in which no antidote or treatment is required and also hospitalization is not required. Example - constipation caused by
- Moderate adverse reaction requires treatment where doses may be modified, but there is no necessity for the therapy to be discontinued. Also, hospitalization may be prolonged for the patient with moderate adverse reaction. Example-venous thrombosis caused by hormonal contraceptive falls under this
- Severe ADR, is potentially life threatening. It is recommended to discontinue the drug therapy and special treatment is required. Example-angioedema caused by
- Lethal ADR that may bring about death either directly or indirectly. Example- Hemorrhage due to anticoagulants [21,22-25].
OBJECTIVE
The aim of the study is to identify the occurrence, types, and management of ADRs, as well as to analyse the causal relationship, severity, and preventability of ADRs in tertiary care super- speciality hospital in Chennai, Tamil Nadu.
METHODOLOGY
The prospective observational study was carried out in Frontier Lifeline Hospital, Chennai. The study was enrolled after the clearance/approval from the Institutional Ethics Committee of Frontier Lifeline Hospital, Chennai [26-28].
STUDY DURATION
The study was carried out for the period of 12 months (Mar 2019-Feb2020).
INCLUSION CRITERIA
- Patient of either sex and any age group
- Patient admitted to hospital due to suspected ADR
- Hospitalise patient who developed ADRs
- ADR caused by contrast media
EXCLUSION CRITERIA
- Patient treated on out-patient department (OPD) basis
- ADR caused by medication error or adverse event
- Patient with drug abuse and medication non compliance
- Patient who developed ADR during the transfusion of blood or blood products and vaccines/medical device
METHODS
Two Pharmacovigilance associates from the regional ADR Monitoring Centre (AMC) were invited to sensitize all our health care professionals on Pharmacovigilance Programme of India, ADR and importance of reporting the same. The clinical pharmacist used to take part in the ward rounds along with physicians, and actively monitor for any ADRs including laboratory investigations if indicated clinically. On intimation of suspected ADRs by the physician or suspicion by clinical pharmacist, the ADR Reporting form was filled up and reported to Pharmacovigilance Programme of India via regional AMC within 24 hrs of time frame, the case was followed up for further details, All the data were kept confidential in respect of the national laws. Patient case notes/files and suspected ADR notification forms were used as main sources of data collection. All the documented ADRs were analyzed for incidence, types of ADRs, drug classes, and individual drug causing reaction, organ system affected, predisposing factors, management and outcome of ADRs. Organ system affected by ADRs were categorized using IBM Micromedex®, Causality assessment was done using WHO-UMC scale, Severity was assessed using modified Hartwig and Siegel, and while preventability was assessed using modified Schumock and Thornton scale [29-34].
To strengthen the awareness of the ADR reporting system posters were displayed. As a reminder, clinical pharmacist highlighted the importance of ADRs reporting system to the nurses during the weekly in- service nursing education class.
RESULTS
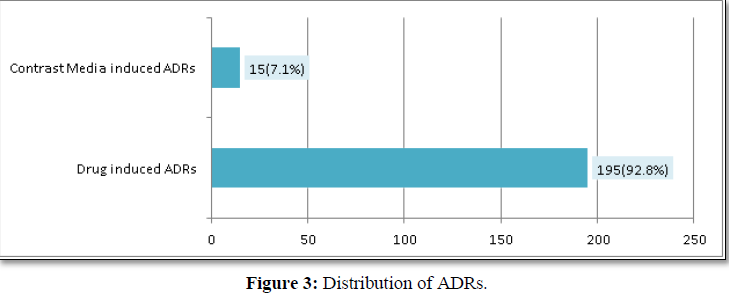
A total of 4,721 patient were admitted during the study period, among them 210 ADR was observed. Of 2,340 angiograms done, 15 developed ADR by Radioactive Contrast Media during the research period [35-38].
GENDER DISTRIBUTION
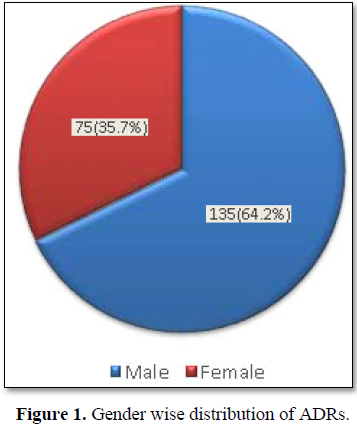
ADRs were detected from patient with a predominance of male gender (64.2%) over females (35.7%) as depicted in Table 1 and Figure 1.
AGE DISTRIBUTION
ADRs were frequently encountered in geriatric patients in the age group of 60-79 years old as shown in Table 2, Figure 2.
The primary objectives of this study are to assess the incidence of medication errors, to evaluate percentage of error prone abbreviations, to assess the incidence of adverse drug reactions.
DISTRIBUTION OF ADRS
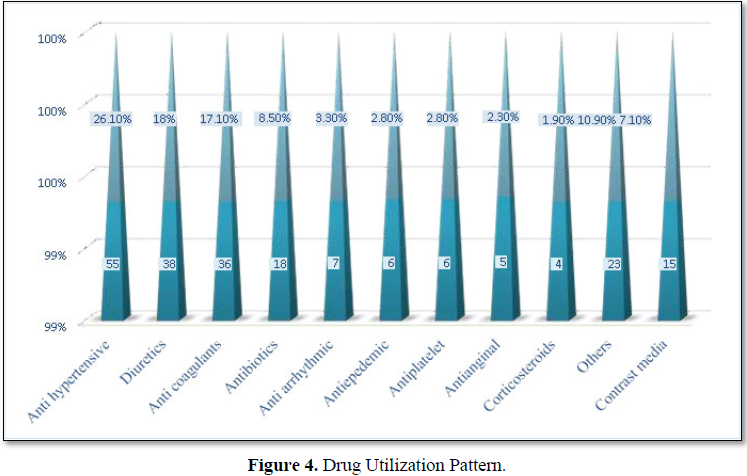
Drug Utilization Pattern
Table 3, Figure 4 indicates that majority of ADRs was encountered by antihypertensive drugs (26%) followed by diuretics (18%), anticoagulants (17%), antibiotics (8.5%), contrast media (15%) [39-45].
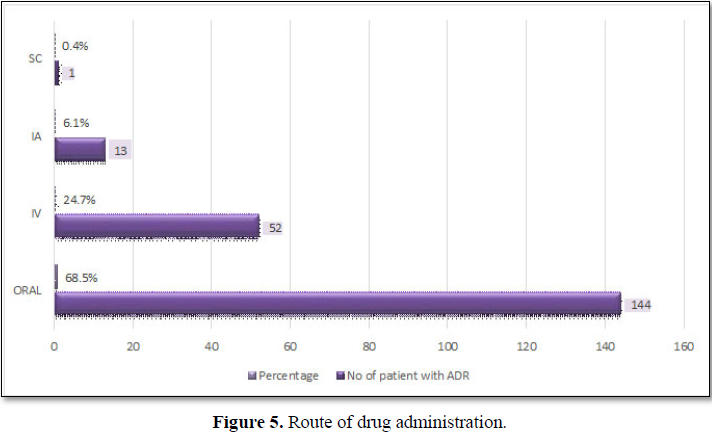
ROUTE OF DRUG ADMINISTRATION
Most of the ADRs was commonly encountered in oral route of drug administration as depicted in Table 4, Figure 5 [46-48].
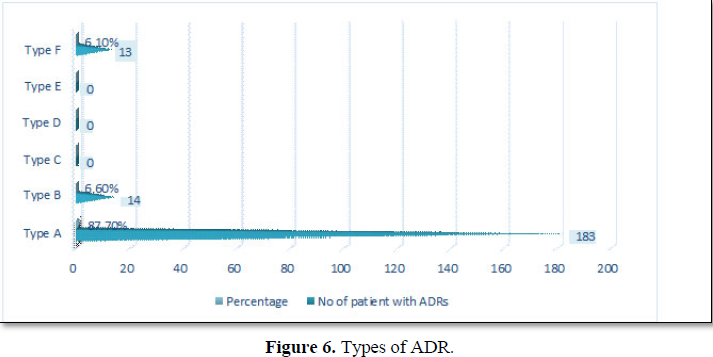
TYPES OF ADR
Type A reaction (87.7%) accounted for majority of report compared to type B (6.6) and type F (6.1) as shown in Table 5, Figure 6 [49].
CLINICAL MANIFESTATION
The most common clinical manifestations of ADRs during the study was hypokalaemia (11.4%) followed by breathlessness (7.6%), hematuria (7.1%) pedal edema (6.1%) and others shown in Table 6 [50-52].
WHO CAUSALITY ASSESSMENT SCALE
Causality assessment was done using WHO-UMC scale. The assessment showed that out of 210 ADRs, (33.3%) were probable, (64.2 %) were possible, (5%) were unlikely as shown in Table 7, Figure 7.
SEVERITY ASSESSMENT BY MODIFIED HARTWIG AND SIEGAL SCALE
According to the modified Hartwig and Siegel scale most of the ADRs reported in the study were mild (52.8%) in nature followed by (39%) were moderate and (8%) were severe as depicted in Table 8, Figure 8.
Preventability Assessment by Modified Schumock and Thornton Scale
Preventability assessment using modified Schumock and Thornton revealed that 115 (54.7%) ADRs were definitely preventable, 76 (36%) ADRs were probably preventable, 19 (9%) were not preventable as shown in Table 9, Figure 9.
ORGAN SYSTEM AFFECTED DUE TO ADRS
In our study we observed that several Organ systems was affected due to ADRs and among them most affected organ system was endocrine metabolic (20) as shown in Table 10, Figure 10.
MANAGEMENT OF ADRS
As a part of management in 87 cases the drug was withdrawn, no changes were done in 16 cases, dose altered in 28 cases and symptomatic treatment was provided in 38 cases as shown in Table 11, Figure 11.
OUTCOME OF ADRS
Adverse drug reaction encountered were treated and the final outcome was measured. About 205 ADRs were recovered and 5 are not known as depicted in Table 12, Figure 12.
HOSPITAL STAY DUE TO ADRS
Table 13, Figure 13 indicates that among 210 reported ADRs 134 cases, were stayed less than 2 days followed by 63 cases, duration of stay was between 3 to 5 days and 13 cases, were stayed more than 6 days.
DISCUSSION
A total of 4,721 patients were admitted during the study period, among them 210 ADRs were detected from patient with a predominance of male gender (64.2%) over females (35.7%). Majority of patients in the study was also males [53,54]. Raujo lobo, et al., have found the incidence of ADRs is unrelated to gender which supports our studies that ADRs did not differ significantly between men and women [54]. ADRs were frequently encountered in geriatric patients in the age group of 60-79 years as shown in Table 1. This group of patient has a very high risk of developing ADR due to age-related changes in pharmacokinetics and pharmacodynamics, increasing burden of comorbidity, polypharmacy, inappropriate prescribing and suboptimal monitoring of drugs. Which is in accordance with the study of Beijer, et al., and Priyadharshini, et al [37,55]. In our study majority of ADR was encountered by antihypertensive drugs (26%) followed by diuretics (38%), anticoagulants (17%), antibiotics (8.5%), contrast media (15%). This study was accordance with Godbharle SB, et al and Mjorndal et al [56]. In the study performed by Mjorndal et al., in a clinic of internal medicine at a Swedish university hospital, cardiovascular drugs were the most common class of drugs involved in the induction of ADRs. Thus, selection of appropriate medicines for patients, enhancing patient adherence with the therapy by selecting medicines of lesser ADR profile, reducing unnecessary economic burden to the patients due to unwanted effects of the therapy could prevent the patient from life threatening complication and hospitalization associated with medication.
In our study majority of ADR was developed by oral administration 144(68.52%). Type A reaction (87.7%) accounted for majority of report compared to type B (6.6) and type F (6.1) which constitute approximately 80% of adverse drug reactions these ADRs are potentially avoidable and often predict-able, which is mainly due to consequence of the drug’s primary pharmacological effect. The most common clinical manifestations of ADRs during the study period was hypokalemia (11.4%) followed by breathlessness (7.6%), hematuria (7.14%), pedal edema (6.19%).
In our study observed that several Organ systems was affected by medication and among them majority was endocrine metabolic (20) followed by hematology (17), cardiovascular (15), GI system (10) and others. As a part of management in 87 cases the drug was withdrawn, no changes were done in 16 cases, dose altered in 28 cases and symptomatic treatment was provided in 38 cases. Adverse drug reactions encountered were treated and the final outcome was measured. About 205 ADRs were recovered and 5 are not known. 134 cases duration of stay was less than 2 days followed by 63 cases stayed between 3 to 5 days and 13 cases stayed more than 6 days.
In order to intensify the validity of the study, causality assessment was done using WHO-UMC scale. The assessment showed that out of 210 ADRs, (33.3%) were probable, (64.2 %) were possible, (5%) were possible. These findings are similar to the study carried out by Javedh Shareef et al and Keezhipadathil J et al [1,53].
On the evaluation of the severity of ADRs by the Hartwig and Siegel severity assessment scale, it was evident that most of the ADRs reported in the study were mild (52.8%) in nature followed by (39%) were moderate and (8%) were severe. No lethal outcomes were observed or produced during the study period and these findings are similar to the previous studies done by Arulmani et al., and Shrivastava et al [50,51].
Assessment of the preventability of the ADRs using modified Schumock and Thornton scale revealed that 115 (54.7%) ADRs were definitely preventable. This study is accordance with Keezhipadathil J et al [1].
CONCLUSION
The present prospective observational study showed that monitoring and reporting of ADRs plays a vital role in medical events. This study shows many factors like age, gender, drug class and drugs with ADR. By implementing the ADR reporting and monitoring system, the pharmacist can easily identify and quantify the risks associated with the use of drugs which promotes drugs safety and better patient care, among health care professionals. Involvement of pharmacist in patient care can also help to detect new and rare ADRs. Monitoring and reporting of ADRs among healthcare professionals should be encouraged as well as creating awareness of ADR reporting among patients can improve quality of life and prevent hospitalization.
- Keezhipadathil J (2019) Evaluation of Suspected Adverse Drug Reactions of Oral Anti-diabetic Drugs in a Tertiary Care Hospital for Type II Diabetes Mellitus. Indian J Pharmacy Practice 12(2): 103-110.
- Sudhakar R, George MK, Yasaswini B, Sundararajan N, Mariyam AS (2016) Adverse drug reactions associated with anti-hypertensive drugs and its management. International Journal of Pharmaceutical Sciences and Research 7(3): 898-913.
- Vikas S, Ramesh M, Rani VN, Thennarasu P, Kannan G (2017) Incidence of diuretics induced adverse drug reactions in an intensive cardiac care unit of a tertiary care teaching hospital. Int J Pharm Sci Res 8(8): 3557-3562.
- Gholami K, Ziaie S, Shalviri G (2008) Adverse drug reactions induced by cardiovascular drugs in outpatients. Pharmacy Practice (Internet) 6(1): 51-55.
- Tutu S, Kant S, Verma AK, Sachan AK, Nath R, et al. (2018) Incidence and pattern of adverse drug reactions (ADRs) in patients treated for Tuberculosis under DOTS at a tertiary care hospital of northern india. Int J Pharm Sci Res 9(11):4950-5.
- Lin RY, Nuruzzaman F, Shah SN (2009) Incidence and impact of adverse effects to antibiotics in hospitalized adults with pneumonia. J Hosp Med 4(2): E7- E15.
- Laskar JI, Chakravarty P, Dewan B (2017) A study on incidence of adverse drug reactions with commonly prescribed drugs and causality assessment in Silchar Medical College and Hospital. Int J Basic Clin Pharmacol 6(5): 1175-1183.
- Schatz S, Weber RJ (2015) Adverse drug reactions. Pharmacy Practice 1(1).
- Palaniappan M, Selvarajan MGS, Subramaniyan G, Dkhar SA, Pillai AA, et al. (2015) Pattern of adverse drug reactions reported with cardiovascular drugs in a tertiary care teaching hospital. J Clin Diagnostic Res 9(11): FC01.
- Abdela J, Assefa A, Shamele S (2019) Prevalence of adverse drug reactions among pediatric patients on antiretroviral therapy in selected hospitals in eastern ethiopia: 8-year retrospective cross-sectional study. J Int Assoc Provid AIDS Care 18: 2325958218823208.
- Hussain A, Aqil M, Alam MS, Khan MR, Kapur P, et al. (2009) A pharmacovigilance study of antihypertensive medicines at a South delhi hospital. Indian J Pharm Sci 71(3): 338-341.
- O'connor MN, Gallagher P, Byrne S, O'mahony D (2012) Adverse drug reactions in older patients during hospitalisation: Are they predictable? Age and ageing 41(6): 771-776.
- Mugoša S, Bukumirić Z, Kovačević A, Bošković A, Protić D, et al. (2015) Adverse drug reactions in hospitalized cardiac patients: Characteristics and risk factors. Vojnosanitetski pregled 72(11): 975-981.
- Chan SL, Ang X, Sani LL, Ng HY, Winther MD, et al. (2016) Prevalence and characteristics of adverse drug reactions at admission to hospital: A prospective observational study. Br J Clin Pharmacol 82(6): 1636-1646.
- Seden K, Kiiza D, Laker E, Arinaitwe WJ, Waitt C, et al. (2018) High prevalence and long duration of nervous system and psychiatric adverse drug reactions in Ugandan patients taking efavirenz 600 mg daily. J Antimicrob Chemother 73(11): 3158-3161.
- Chandrashekhar VM, Harikrishna A, kumar P, Hemanthkumar N, Chandrakanth M (2016) Adverse drug reaction monitoring and reporting at h.s.k hospital and research center-bagalkot. Indian J Pharm Prac 9(1): 49-56.
- Pendota S, Surabhineni SAK, Katnapally AS, Porandla D, Beemreddy SK (2017) Classification and applying pharmacovigilance principles to study adverse drug reaction and its management. Int J Basic Clin Pharmacol 6(11): 2537-2544.
- Cahir C, Curran C, Byrne C, Walsh C, Hickey A, et al. (2017) Adverse Drug Reactions in an Ageing Population (ADAPT) study protocol: A cross-sectional and prospective cohort study of hospital admissions related to adverse drug reactions in older patients. BMJ open 7(6).
- Mukherjee S, Sen S, Chatterjee SS, Era N, Ghosal M, et al. (2015) Tripathi SK. Adverse drug reaction monitoring of antidepressants in the psychiatry outpatient department at a tertiary care teaching hospital in India: A cross-sectional observational study. Eur J Psychol Edu Stud 2(1): 14.
- Giardina C, Cutroneo PM, Mocciaro E, Russo GT, Mandraffino G, et al. (2018) Adverse drug reactions in hospitalized patients: Results of the FORWARD (facilitation of reporting in hospital ward) study. Front Pharmacol 9: 350.
- Kalyani SSA, Srihitha P (2017) An epidemiological study on adverse drug reactions in indian population: Meta-Analysis. Int J Pharm Clin Res 9(10): 654-659.
- Patel TK, Thakkar SH, Sharma DC (2014) Cutaneous adverse drug reactions in Indian population: A systematic review. Indian Dermatol Online J 5: S76.
- Singh A, Dwivedi S (2017) Study of adverse drug reactions in patients with diabetes attending a tertiary care hospital in New Delhi, India. Indian J Med Res 145(2): 247-249.
- Gor AP, Desai SV (2008) Adverse drug reactions (ADR) in the inpatients of medicine department of a rural tertiary care teaching hospital and influence of pharmacovigilance in reporting ADR. Indian J Pharmacol 40(1): 37-40.
- Tandon VR, Mahajan V, Khajuria V, Gillani Z (2015) Under-reporting of adverse drug reactions: A challenge for pharmacovigilance in India. Indian J Pharmacol 47(1): 65-71.
- Rehan HS, Sah RK, Chopra D (2012) Comparison of knowledge, attitude and practices of resident doctors and nurses on adverse drug reaction monitoring and reporting in a tertiary care hospital. Indian J Pharmacol 44(6): 699-703.
- Kalaiselvan V, Thota P, Singh GN (2016) Pharmacovigilance programme of india: Recent developments and future perspectives. Indian J Pharmacol 48(6): 624-628.
- Mukherjee S, Era N, Saha B, Tripathi SK (2017) Adverse drug reaction monitoring in patients on antiretroviral therapy in a tertiary care hospital in Eastern India. Indian J Pharmacol 49(3): 223-228.
- Piparva KG, Buch JG, Chandrani KV (2011) Analysis of adverse drug reactions of atypical antipsychotic drugs in psychiatry OPD. Indian J Psychol Med 33(2):153-157.
- Wadhwa T, El Sheikh SG, Rao PG (2018) Monitoring and reporting of adverse drug reactions due to cardiovascular drugs in patients admitted to a secondary care hospital in Northern Emirate-a prospective surveillance study. Indian J Pharmacy Practice 11(2): 71-78.
- Kodati D, Tirumala S, Kantheti RK, Thumma JP (2019) A retrospective study on the adverse effects of chemotherapy in breast cancer-a multicenter study. Indian J Pharmacy Practice 12(2): 111-116.
- Dhikav V, Singh S, Anand KS (2004) Adverse drug reaction monitoring in India. J Indian Acad Clin Med 5(1): 27-33.
- Upadhyaya HB, Vora MB, Nagar JG, Patel PB (2015) Knowledge, attitude and practices toward pharmacovigilance and adverse drug reactions in postgraduate students of Tertiary Care Hospital in Gujarat. J Adv Pharm Technol Res 6(1): 29-34.
- Akhideno PE, Fasipe OJ, Isah AO (2018) The incidence and prevalence of adverse drug reactions among medical inpatients in a Nigerian University Teaching Hospital. J Curr Res Scientific Med 4(2): 86-93.
- Torwane NA, Hongal S, Gouraha A, Saxena E, Chavan K (2015) Awareness related to reporting of adverse drug reactions among health caregivers: A cross-sectional questionnaire survey. The Journal of National Accreditation Board for Hospitals & Healthcare Providers 2(1): 23-29.
- Rende P, Paletta L, Gallelli G, Raffaele G, Natale V, et al. (2013). Retrospective evaluation of adverse drug reactions induced by antihypertensive treatment. J pharmacol pharmacother 4(Suppl1): S47-S50.
- Priyadharsini R, Surendiran A, Adithan C, Sreenivasan S, Sahoo FK (2011) A study of adverse drug reactions in pediatric patients. J pharmacol pharmacother 2(4): 277-280.
- Sharma S, Swamy S, Bhambhani A, Nadig P (2018) Adverse drug reactions attributed to fondaparinux and unfractionated heparin in cardiovascular care unit: An observational prospective pilot study in a tertiary care hospital. J Pharm Bioallied Sci 10(2): 90-95.
- Wilson V, Amma V (2015) Prospects of consumer-initiated adverse drug reaction reporting in cardiovascular pharmacovigilance. Journal of the Practice of Cardiovascular Sciences 1(1): 54-57.
- Mateti UV, Nekkanti H, Vilakkathala R, Rajakannan T, Mallayasamy S, et al. (2012) Pattern of angiotensin-converting enzyme inhibitors induced adverse drug reactions in South Indian teaching hospital. N Am J Med Sci 4(4): 185-189.
- Amin S, Shah S, Desai M, Shah A, Maheriya KM (2018) An analysis of adverse drug reactions in extremes of age group at tertiary care teaching hospital. Perspect Clin Res 9(2): 70.
- Desai CK, Iyer G, Panchal J, Shah S, Dikshit RK (2011) An evaluation of knowledge, attitude, and practice of adverse drug reaction reporting among prescribers at a tertiary care hospital. Perspect Clin Res 2(4): 129-136.
- Elnagar BMI (2017) Prevalence and Extent of Adverse Drug Reactions in Sudanese Patients in Highly Active Anti-Retroviral Therapy Regimens. Int J Pharmacovigil 2(2): 12.
- Singh A, Prasad R, Balasubramanian V, Gupta N, Gupta P (2015) Prevalence of adverse drug reaction with first-line drugs among patients treated for pulmonary tuberculosis. Clin Epidemiol Glob Health 3: S80-S90.
- Hagos L, Fessehaye S, Anand IS (2019) Nature and prevalence of adverse drug reaction of antiretroviral medications in Halibet National Referral Hospital: a retrospective study. BMC Pharmacol Toxicol 20(1): 24.
- Haider N, Mazhar F (2017) Factors associated with underreporting of adverse drug reactions by nurses: A narrative literature review. Saudi J Health Sci 6(2): 71.
- Amalia L, Anggadireja K, Aprami TM, Septiani V (2016) Prevalence of adverse drug reactions in cad stemi patients treated in the cardiac intensive care unit at the public hospital in bandung, Indonesia. Sci Pharm 84(1): 167-179.
- Lucca JM, Ramesh M, Ram D, Kishor M (2016) Incidence and predictors of adverse drug reactions caused by drug-drug interactions in psychiatric patients: An empirical study. Trop J Med Res 19(1): 29-35.
- Akhideno PE, Fasipe OJ, Isah AO, Owhin OS, Adejumo OA (2019) Pattern of medications causing adverse drug reactions and the predisposing risk factors among medical in- patients in clinical practice: A prospective study. J Med Sci 39(1): 18-27.
- Arulmani R, Rajendran SD, Suresh B (2008) Adverse drug reaction monitoring in a secondary care hospital in South India. Br J Clin Pharmacol 65: 210-216.
- Shrivastava M, Uchit G, Chakravarti A, Joshi G, Mahatme M, et al. (2011) Adverse drug reactions reported in Indira Gandhi Government Medical College and Hospital, Nagpur. J Assoc Physicians India 59: 296-299.
- Javedh S, Jennifer F, Laxminarayana S, Shifaz AK (2016) A Study on adverse drug reactions in hospitalized patients with diabetes mellitus in a multi-specialty teaching hospital. Asian J Pharm Clin Res 9(2): 114-117.
- Lobo MGA, Pinheiro SM, Castro JG, Momenté VG, Pranchevicius MC (2013) Adverse drug.reaction monitoring: support for pharmacovigilance at a tertiary care hospital in Northern Brazil. BMC Pharmacol Toxico 14(1): 5.
- Beijer HJ, De Blaey CJ (2002) Hospitalisations caused by adverse drug reactions (ADR): A meta-analysis of observational studies. Pharm World Sci 24(2): 46-54.
- Singh P (2017) Adverse drug reactions at adverse drug reaction monitoring center in Raipur: Analysis of spontaneous reports during 1 year. Indian J Pharmacol 49: 432-437
- Godbharle SB, Padwal SL (2019) Study of adverse drug reactions in a tertiary care hospital. Int J Basic Clin Pharmacol 8(9): 76.