3662
Views & Citations2662
Likes & Shares
Many patients who get chemotherapy need continuous delivery over an extended infusion time and require specialized pumps for the outpatient setting. There are a few types of pumps that can deliver chemotherapy in this setting. This paper will focus on an overview of elastomeric pumps and continuous ambulatory delivery device (CADD) pumps. One of the most common medications used is 5-flourouracil for an extended infusion. There are many aspects on the nursing, pharmacy and patient side that go into making this successful. This paper will also discuss preparing pumps, administering pumps and counseling points for patients with these pumps along with toxicities and adverse effects of a long term infusion of 5-flourouracil.
Keywords: Chemotherapy, Pump, 5-FU, 5-Flourouracil, Continuous chemotherapy
INTRODUCTION
Continuous ambulatory delivery devices (CADD pumps) are made to supply a continuous dose of medication to patients requiring around the clock infusions in cases such as anal carcinoma, colorectal cancer with metastasis in the liver, etc. These devices allow patients to be able to receive their IV medications and not be required to stay in an infusion center or be hospitalized for their infusion. These devices have multiple uses to help decrease patient time burden and also healthcare work burdens. CADD pumps require the patient to carry the electric pump as well as the IV fluid bag, preferably in a self-containing bag. These pumps allow healthcare personnel to program dosing schedules, such as scheduled bolus, tapering boluses, etc. Elastomeric pumps deliver a low steady dose of medication until it is empty. This article will discuss how these pumps are used, and their benefits and risks [1].
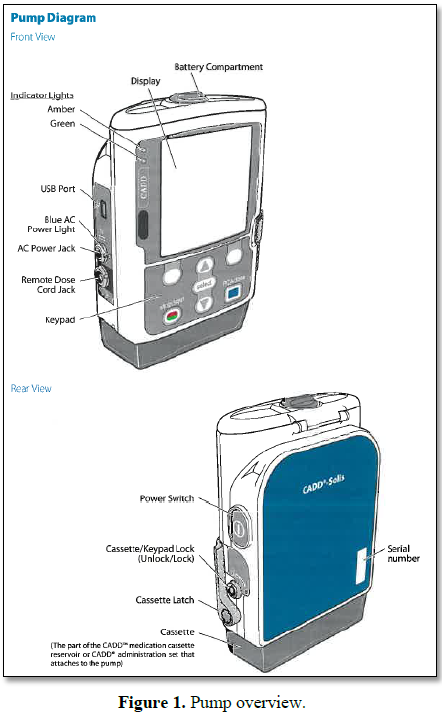
Smith Medical makes a CADD pump that has multiple uses. It can deliver medicine in low bolus doses, like those used in patient controlled analgesia (PCA) systems, or larger continuous dosing. It also has settings for intermediate bolus delivery dosing, where it can be programmed to give scheduled large doses on a schedule. Other programming steps allow for step therapy, where dosing is increased until a certain amount and then decreases or a variation of step therapy via tapering up and tapering down a dose. These pumps do not have fluid restrictions on what they require in their IV fluid bag. The electronic pump has two connections, one that attaches to the patient’s IV catheter and one that connects to the IV bag. The pump itself has a few safety mechanisms built into its programming to allow patient safety, such as air bubble warnings or battery detachment. This pump when in its PCA mode doses by milligrams per milliliter and milliliters per hour. It is always important to verify the pump settings, and also how the medication is being delivered [1].
Making and Using Electronic Pumps
When making the IV bag for your patients, you should always follow your sterile compounding and chemotherapy protocols. While doing so compound your IV fluid bags as needed to hold the sufficient amount of drug for the whole infusion. Once compounded and ready for delivery, verify that the pump is set for continuous infusion for the correct flow rate to reach the total time required for infusion. Under the continuous infusion settings it can be changed to 0.1 mL/h to 500 mL/h in 0.1 mL/h increments. It has a delay setting of delivering 0.1 mL/h to 10 mL/h. Again verify that the calculation is correct that allows sufficient fluid and drug concentration for the whole infusion time.
Here is an example: A patient comes to receive their IV bag of fluorouracil. They are dosed at 1,000 mg/m2/day for a continuous day 1-4 of a 3 week cycle. Previous calculations showed the patient has a BSA of 1.40 m2. The patient will need to receive 1,400 mg daily over a continuous infusion daily for 4 days. The patient will need to have an IV bag with 5,600 mg in an IV bag. The compounded IV bag will be 500 mL containing the 5,600 mg.This concentration is 11.2 mg/mL. This means that the patient will need to receive 125 mL over 24 h. This comes out to the patient receiving 5.2 mL/h.
1,000 mg/m2/day * 1.4 m2=1,400 mg/day
1,400 mg/day * 4 days=5,600 mg
Compounded into a 500 mL IV bag. Final concentration 5,600 mg/500 mL=11.2 mg/mL
1,400 mg/day divided by 1 mL/11.2 mg=125 mL/24 h=5.2083 mL/h rounded to the nearest 0.1
Once infusion time and concentrations are correct and set in the machine, both the pump and the fluid bag should be secured into its carrying case where it will not kink any tubing and be protected from any environmental factors. Your nursing team is an immense help to you if you are not familiar with using the pumps [1].
Elastomeric Pumps
Baxter International makes two different nonelectronic elastomeric pumps that can be used for a short time, up to 5 h or long intervals, up to 7 days. It is important to use the right pump for the occasion as there are two type of pumps; infusors and intermates. Both pumps work the same but have different indications and length of treatment times. Elastomeric pump infusors have long infusion times and are designed for ambulatory infusion of IV chemotherapy, pain management and chelation therapies. Elastomeric pump intermates are used for antibiotic/antiviral infusions. These elastomeric pumps work differently than in-patient infusions that require an electronic machine pump that controls flow rates. They work by slowly “deflating” a medication-filled balloon directly into the IV line. There are different sized bags that allow for different infusion times and different flow rates. Using the correct bag and solution decreases the need for patients returning to infusion centers and also adverse events, such as medication overdosing. Infusors and intermate pumps should never be re-used but properly disposed.
The Elastomeric infusors require the use of dextrose 5% water and are used for long term infusions, whereas, the elastomeric intermates require the use of normal saline and are for shorter time periods. Using the wrong solution in the bag will change the flow rate approximately by 10%. Access needles also affect the rate of infusion, thinner gauge needles will decrease infusion flow rates and wide gauges will increase flow rates. Temperature and pump placement are other large flow rate factors. As a general rule of thumb, keep the pump placement level with the Luer Lock connector. Moving the pump up or down, for every inch, can increase or decrease flow rate by 0.5%, respectively. Once the drug is attached to the Luer Lock connector, the infuser can be attached to the patient. The infusor should be placed on the torso so that the bag can stay within a 92°F range. The intermates should rather be attached to a limb to achieve 70°F, such as a leg or arm, whichever is level to the luer lock and does not inhibit patient movement, thus defeating the goal of ambulation while receiving an elastomeric pump (Figure 1) [2].
Then, the pharmacist will need to determine how long of an infusion time is going to be required to pick out the correct infuser pump. These are color coordinated to help reduce drug errors; however, there have been incidents of using the wrong pump because of the color coordination, so verify as well by reading the package what size of elastomeric pump you have. Each pump has a different flow rate and maximum volume carrying load. When making an elastomeric pump, the balloon itself is empty. It will need to be filled to its ‘nominal’ volume. The balloon is prepared to hold more than the given nominal volume if you accidentally overfill it. If you do not fill the pump to the nominal volume, the balloon pump will push the drug out too quickly [2].
Making the Elastomeric Pump
The manufacturers give very detailed guidelines on how to make the pump. There are two cap ends. One is the fill port, which puts medicine directly into the balloon and the winged Luer Cap that attaches to the patient IV catheter. Remember the maximum volume is not the same as the nominal volume. The nominal volume is how much the balloon need to deliver the correct flow rate for the patient, it is very important that the balloon is filled to at least the nominal volume, but not over the maximum volume.
1. Calculate how much diluent and drug liquid is required.
2. Remove the tape and verify the winged luer cap is secured.
3. Remove the port cap and inject diluent gently into the balloon reservoir.
Note, you do not need the needle to do this, as it will damage the port!
4. Inject all the diluent, and this may become very difficult, so you may need to use the hood’s table to help you inject the rest of the diluent by placing the plunger directly on the table and pushing the syringe and pump down.
5. Remove diluent syringe once diluent is in reservoir and re-cap.
6. Uncap the winged luer cap, the part that attaches to the patient catheter and let the diluent come down the tubing. Let 3 drops of diluent fall onto a alcohol wipe.
7. If this happens, recap and repeat the filling steps with the drug until the elastomeric pump is ready to be delivered to the patient.
8. Close the filling port and the winged luer port caps. Follow drug protection procedures, such as protecting from light, etc., and then it is ready for the infusion.
9. If the diluent did not flow out the opened winged luer port, you will need to use a separate syringe that will be attached to the winged luer port to reach a vacuum to pull the diluent down. A 10 mL syringe should be sufficient to do this, once this happens go back up to letting it drop onto the alcohol wipe and continue making.
Calculations for using the elastomeric pumps will be similar to that of the electric pumps except you are limited by infusing flow rates and reservoir sizes [2].
Teaching Points for the Infusion Nurses
Most hospital nurses will know how to deal with CADD pumps. Those nurses that are not familiar with elastomeric pumps should be shown how they work and instructed on how long elastomeric pumps will infuse medication [1].
● Verify that there is liquid at the end of the tubing when the winged Luer cap is removed [1].
● Flush the IV line. Infusor elastomeric pumps should have their Luer Lock connector taped to the patient skin [1].
● Unclamp the catheter [1].
● Place pump in carrying bag and have the bag with pump attached or placed into something that will protect the bag [1].
● (For Elastomeric pumps) The top of the pump needs to be level with the luer lock connector [2].
● (for Electric CADD pumps) Make sure the batteries are good and the infusion flow rate and duration is programmed correctly before the patient leaves [1].
Teaching Points for the Patients
● (For Elastomeric Pumps)When pumps are empty there will be 8 indicator pumps, 4 on each side, and a deflated bag [2].
● Keep the tubing from being kinked or pinched. This will slow or even stop medicine from flowing through the IV catheter [2].
● Avoid hot/cold temperature extremes, and keep out of direct sunlight [2].
● It is safe to use the pump while flying in pressurized airplane cabins [2].
● If you have pets, ensure that it is protected from chewing and playing [2].
● (For Electric pumps) Verify you have good batteries running the machine or that the rechargeable battery for the machine is in working order [1].
● (For electric pumps) when an alarm goes off from the pump, read the alarm and follow what instructions the infusion team has told you to do, or all the infusion team [1].
● You can still shower, sleep, and do normal activities with the pumps.
● Keep the pump from getting wet, by placing it in an extra plastic bag or outside of the shower/bath [2].
● (For Elastomeric pumps) When sleeping, for infusions that require the patient to wear the pump during evening hours, keep the top of the pump level with the Luer Lock Connector “Port”. You can lay it down on its side and place it under your pillow if needed [2].
Adverse Reactions to Using the Pumps
Patients that experience adverse reactions while using the pump will be because of the pump is either filled with a higher fluorouracil concentration or is delivering the drug too fast. There have been reports from previous years of patients receiving up to 5 times the desired dose of medication. Patients that have these types of situations should be hospitalized, even if the prognosis is good. ISMP reports of a case where the patient received 5 times the desired amount of 5-FU because of a miscalculation by the pharmacist and another incident where the pharmacist infused a 46 h regimen in 2 h by using the wrong pump. Both of these patients had to be hospitalized, given an antidote to 5-FU (uridine triacetate formerly called vistonuridine/vistogard) and monitored. Review and follow your hospital’s procedure for drug overdoses/toxicities when any patient is using an ambulatory pump in the chance occurrence that a mistake happens [3].
Adverse Reactions with Fluorouracil
The most common adverse reactions to fluorouracil are diarrhea, nausea and vomiting, mouth sores, taste changes and poor appetite, watery eyes, photosensitivity and pancytopenia [4,5]. These reactions can occur shortly after infusion and can occur even 2 weeks after infusion. Often times, pancytopenia occurs 10-14 hours after infusion. An uncommon side effect of fluorouracil is Palmar-Plantar erythrodysesthesia. This is where the palms and soles develop a rash, swell, peel and become painful. In most cases it is mild, and is dose dependent. It can occur up to 5-6 weeks after starting fluorouracil [5].
To help mitigate and decrease the chance of these reactions from occurring patients should stay well hydrated, and chew on a few ice chips during the continuous infusion to decrease the chance of mouth sores. They should also avoid groups of people and/or wear a mask when around those that have an active infection. Measures to help decrease diarrhea, such as proper nutrition with or without anti-diarrheal medication can be used too. To help decrease Palmar-Plantar erythrodysesthesia, patients should keep their skin moist and and pliable and avoid excess friction and heat exposure to hands and feet [5].
An adverse reaction is not reason to give patient the antidote, Vistogard or Xuriden. Adverse reactions need to be monitored and treated symptomatically. The only time these patients will need Vistogard is in the event of an overdose or a toxicity reaction. Overdoses occur as stated in the previous section of giving the patient too much drug during the correct infusion time or total infusion over too short of a time. Vistogard is extremely expensive and we should do everything in our power to prevent the need for its use, but be willing to dispense if the need for it arises. Follow the package insert for Vistogard for adult toxicities and Xuriden for accidental pediatric toxicities/overdosing [4].
CONCLUSION
We are a part of a medical team and should help teach everyone on our team, including the patients their role in using these pumps. The use of the CADD pump or the elastomeric pump can be beneficial to our long term chemotherapy infusion patients. We must use the correct materials and safety precautions when we make and dispense it to our patients, this will prevent any accidental poisoning to our team, and patient. Preventing overdoses, such as infusing too quickly or giving too much drug is a major concern while using these pumps and we should constantly check ourselves to verify we are using the correct supplies and also the machines we use are set correctly.
1. (2012) Smiths-Medical: CADD-SOLIS VIP ambulatory infusion pump technical manual. Model 2120. Smiths-Medical ASD. Inc. St. Paul, MN, USA.
2. (2010) Baxter elastomeric pump: A clinician’s guide. Baxter Corporation, Mississauga, Ontario.
3. Institute for Safe Medication Practices (2015) Accidental overdoses involving fluorouracil infusions. Accessed online on 7/1/2016.
4. Wolters Kluwer Clinical Drug Information, Inc. (2016) Uridine triacetate and fluorouracil package inserts: Lexi-Comp. Accessed at online.lexi.com.
5. (2016) Fluorouracil: Drug information. Accessed on 7/4/2016.
QUICK LINKS
- SUBMIT MANUSCRIPT
- RECOMMEND THE JOURNAL
-
SUBSCRIBE FOR ALERTS
RELATED JOURNALS
- Journal of Infectious Diseases and Research (ISSN: 2688-6537)
- Journal of Oral Health and Dentistry (ISSN: 2638-499X)
- Advance Research on Endocrinology and Metabolism (ISSN: 2689-8209)
- Journal of Pathology and Toxicology Research
- Journal of Allergy Research (ISSN:2642-326X)
- International Journal of Internal Medicine and Geriatrics (ISSN: 2689-7687)
- International Journal of Diabetes (ISSN: 2644-3031)